Medicare Coverage of Major Pain Procedures May End
One in five Americans with chronic pain could soon lose access to evidence-based interventions that have been around for decades.
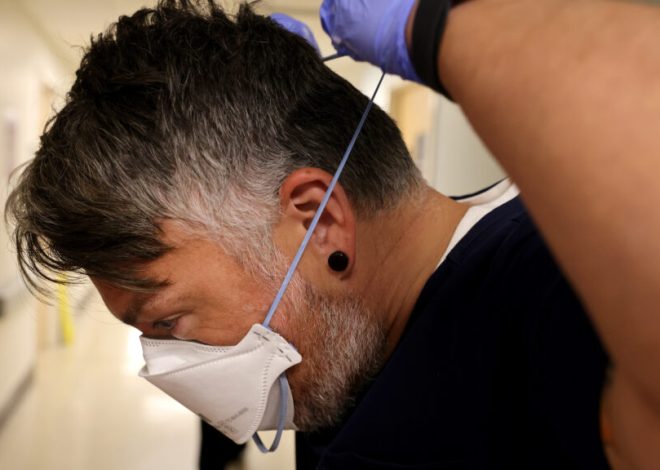
Impending changes in Medicare coverage threaten access to local anesthetic blockade or “peripheral nerve block” procedures. Medicare administrative providers across the country have recently proposed eliminating coverage of these minimally invasive, non-opioid treatment options for chronic pain disorders. If approved, these coverage changes could drive patients back to opioids, exacerbating the overdose epidemic in the United States and forcing patients to needlessly resort to invasive and costly surgical procedures.
Chronic pain is a leading cause of disability in the United States. It is associated with depression, substance use disorders, an economic burden of $722.8 billion in medical costs per year, and loss of productivity. Chronic pain diagnoses are more common among veterans, women, adults living in poverty, and those residing in rural areas.
The challenge of striking a balance between treating chronic pain and combating the opioid overdose epidemic remains one of the leading public health challenges in the United States. Guidelines published by the American Society of Anesthesiologists Task Force on Chronic Pain Management emphasize the importance of a multimodal approach to therapy including non-opioid analgesics, physical and psychological therapy, and minimally invasive procedures.
Peripheral nerve blocks are minimally invasive procedures that are well tolerated by patients. They are considered relatively inexpensive procedures, especially when compared to alternatives such as orthopedic surgery under general anesthesia or hospitalizations for severe pain requiring treatment with intravenous opioid medications. These interventions have broad applications for patients suffering from conditions that cause chronic pain, such as headaches and trigeminal neuralgia. Trigeminal neuralgia is a condition characterized by unpredictable attacks of facial pain so severe that it is associated with depression and suicidal ideation. These patients frequently report immediate pain relief after a peripheral nerve block, with the majority of patients experiencing a greater than 50% reduction in pain, which can last for several months and allow patients to return to work and care for their children.
Similarly, peripheral nerve blocks have been shown to be effective both in reducing pain during acute migraine attacks and in preventing chronic migraines. Migraine patients who undergo occipital nerve blocks experience fewer headache days per month, which may lead to reduced analgesic use (including opioids) and reduced migraine-associated disability. These procedures are also used for patients with chronic pelvic pain, adhesive capsulitis (frozen shoulder), knee osteoarthritis, and complex regional pain syndrome. If patients experience pain relief from a peripheral block, some undergo placement of peripheral nerve stimulators or denervation procedures that reduce or eliminate the nerve’s ability to transmit pain signals. However, diagnostic peripheral nerve blocks should precede these interventions. Symptom relief from these procedures can last from several months to several years.
Yet on September 25, five of the 12 Medicare Administrative Contractors (MACs) in the United States, representing 24 states, announced plans to significantly restrict Medicare coverage for peripheral nerve blocks. Medicare contractors are private insurers that process claims for Medicare Parts A and B. Acting as intermediaries between the federal government and Americans insured by Medicare, these private entities make more than 90% of coverage decisions in the United States by issuing local coverage determinations (LCDs). These policies define what procedures and medications are “reasonable and necessary” for Medicare coverage and influence other government payers and commercial insurance programs. Although this change would initially only affect the 24 states governed by the five MACs, other states could follow suit, and often private insurers follow as well.
Under the proposed LCDs, chronic pain procedures would be limited to three steroid injections for median nerve pain, two steroid injections for Morton neuroma, and radiofrequency neurolysis for trigeminal neuralgia. All other peripheral nerve blocks and denervation procedures would not be covered. Unless MACs want more Americans unable to work, addicted to opioids, and in pain, it’s hard to understand their motivation here. Eliminating coverage for peripheral nerve blocks will not result in significant savings for these patients and could lead to more frequent emergency room and clinic visits, increased use of opioids and other pharmacologic interventions, or more time spent on disability, ultimately increasing direct and indirect healthcare costs in the United States.
These coverage changes have raised concerns among many professional groups, including the American Society of Regional Anesthesia and Pain Medicine and the American Society of Interventional Pain Physicians, which have criticized LCDs’ extremely restrictive criteria for evaluating the effectiveness of peripheral nerve blocks. The Medicare Administrative Contractor websites state that the new policy was developed to “incorporate new procedures and literature.” However, LCD screens exceed the standards of evidence used even in Cochrane reviews, which are known to reject more than 90% of available treatments.
The analysis also ignores the ethical challenges of conducting randomized controlled trials, particularly for procedures with decades of clinical use and established benefits.
Additionally, the policies include procedures that do not fit the definition of peripheral nerve blocks, stellate ganglion blocks, and cervical sympathetic nerve blocks, as well as three irrelevant diagnostic procedure codes, raising questions about the expertise of those writing the LCDs. Despite guidelines from the 21st Century Cures Act of 2016 calling for increased transparency throughout the LCD process, it is difficult to determine the individuals and associated conflicts of interest involved in the authorship of these materials. Only two out of five MACs list a doctor on the LCD website, and one of those two is an OB-GYN with no relevant advanced training.
Physicians and advocates concerned about the proposed coverage changes should contact their state Senate and House health policy representative committees, register and provide expert opinions at contractor meetings, and share their clinical expertise during open public comment periods through November 8.
Tricia Pendergrast, MD, is an anesthesiology resident at the University of Michigan. You can find her on TikTok.
Firm Law
Agen Togel Terpercaya
Bandar Togel
Sabung Ayam Online
Berita Terkini
Artikel Terbaru
Berita Terbaru
Penerbangan
Berita Politik
Berita Politik
Software
Software Download
Download Aplikasi
Berita Terkini
News
Jasa PBN
Jasa Artikel