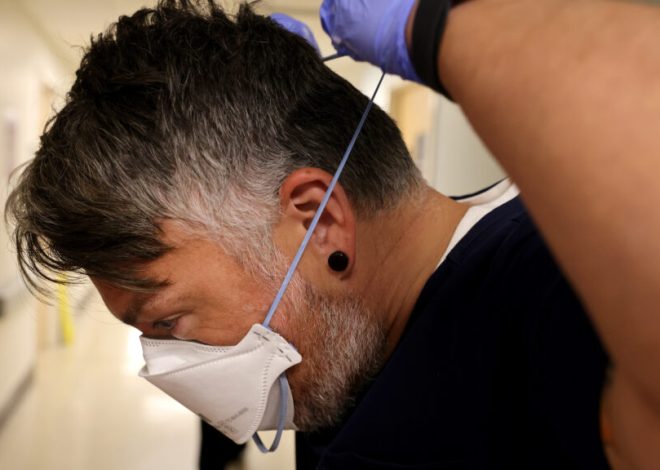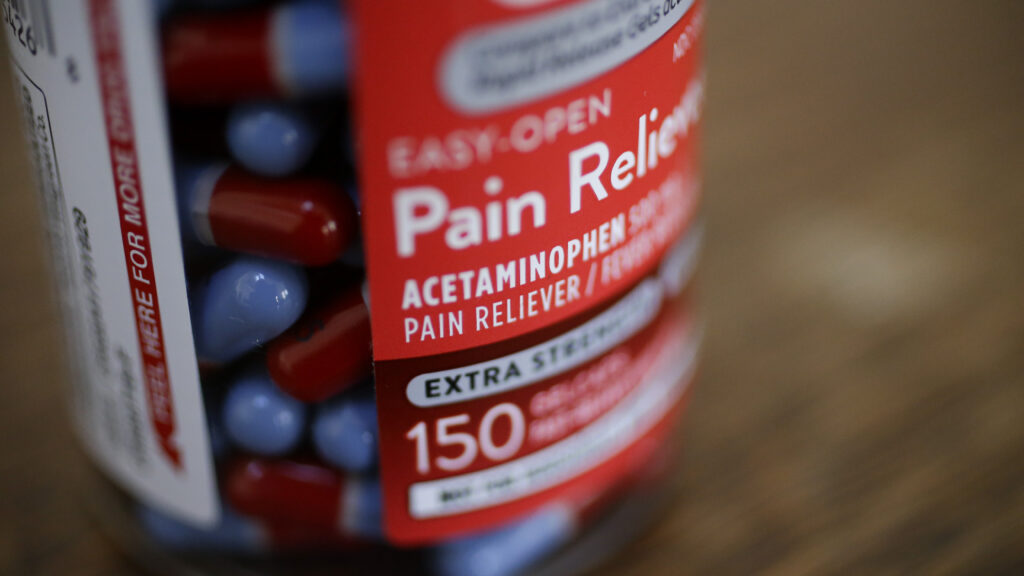
Lancet Study: Using Tylenol During Pregnancy Does Not Cause Autism
Taking acetaminophen during pregnancy is not likely to increase the risk of having a child with autism, ADHD or intellectual disability, according to a new study released Friday.
Researchers across Europe re-examined evidence from several studies investigating the link between these conditions and the use of paracetamol – called acetaminophen in the US – and found that these purported associations broke down after controlling for confounding factors.
Acetaminophen, the active ingredient in Tylenol, has long been a first-line medication to relieve pain or fever in pregnant people. The scientific literature shows that this practice is unlikely to change, said co-author Asma Khalil, professor of obstetrics and maternal-fetal medicine at St. George’s Hospital, University of London.
“The message is really clear,” Khalil said. “Paracetamol remains a safe option during pregnancy when taken as directed, for the length of time needed, in the correct dose.”
Independent health experts praised the study’s methods and findings, which are a stark departure from recommendations made by President Trump and top health officials in September, when they said acetaminophen should only be used when absolutely necessary during pregnancy and launched a nationwide public information campaign to inform doctors and families of the alleged risk. Their announcement is part of their attempt to find the cause of autism, which decades of research has already linked to primarily genetic factors.
It is unlikely that the results of this new study, published in The Lancet, will change these recommendations. Health and Human Services officials said the study does not refute other researchers’ claims.
“Many experts have expressed concern about the use of acetaminophen during pregnancy, including Dr. Andrea Baccarelli, dean of the Harvard School of Public Health,” said HHS spokesperson Andrew Nixon.
The American government is an exception in discouraging the use of acetaminophen: the American College of Obstetricians and Gynecologists, its British counterpart the Royal College of Obstetricians and Gynecologists, as well as the European Medicines Agency continue to recommend this drug as first-line treatment for pain and fever in pregnant women.
The position of US health authorities that exposure to acetaminophen during pregnancy is associated with autism spectrum disorders has prompted European researchers to re-examine the available evidence. Acetaminophen is an essential tool for doctors, the go-to drug for use during pregnancy, because other commonly available pain relievers, such as Advil (ibuprofen), and opioid medications can put the fetus at risk of kidney damage, premature birth, or even stillbirth. Acetaminophen is not only a pain reliever for pregnant women, it also reduces fever which can increase the risk of birth defects.
Scientists have had ample time to study the potential adverse effects of acetaminophen, a drug first used clinically in 1893, so much so that “there may be more reviews of acetaminophen studies than there are actual studies of acetaminophen with primary data,” joked Brian Lee, a professor of epidemiology at Drexel University. In general, they found that the benefits of acetaminophen outweigh the risks associated with its use. Why, then, did Khalil and his team add another meta-analysis to the big pile of studies?
Lee and other experts view the Lancet article as a direct rebuke of a meta-analysis published in 2025 and co-authored by Baccarelli. Both articles analyze many of the same studies, but the 2025 review came to a radically different conclusion, finding “significant links” between acetaminophen use during pregnancy and increased risks of conditions like autism or ADHD. Baccarelli’s article was cited by senior health officials in September, saying the dean had established a “causal relationship” between the drug and these side effects.
Baccarelli has so far declined to comment on health officials citing his work to urge caution in the use of acetaminophen, or the testimony he gave to forcefully assert a link between acetaminophen use during pregnancy and conditions like autism. A spokesperson for the Harvard TH Chan School of Public Health said Baccarelli was not available to discuss the new Lancet study.
The authors of the new Lancet study sorted thousands of published articles into 43 studies based on the risk of “bias,” or how well the articles’ study designs and protocols accounted for confounding factors, such as genetics. The authors prioritized studies in which a mother took acetaminophen during one pregnancy but not another. If autism or other neurodevelopmental issues were associated with an environmental factor such as taking Tylenol, then researchers would discover this difference in siblings’ neurodevelopmental outcomes.
But that’s not what the researchers found, particularly when evaluating data from two notable studies from Sweden and Japan, which used this method on massive datasets. When researchers conducted a meta-analysis of these and 15 other articles, they found no association between maternal acetaminophen use and increased risk of autism, ADHD, or intellectual disability.
David Mandell, professor of psychiatry at the Perelman School of Medicine at the University of Pennsylvania, applauded the Lancet study’s robust design and commitment to controlling for confounding variables, calling it a “pretty strong rebuke” of Baccarelli’s paper, which devalued sibling control studies in its analysis.
“Even though there are scientific best practices for conducting reviews and meta-analyses, they are still largely the result of subjective interpretation,” Lee said. “Beauty is in the eye of the beholder, but compared to Prada et al.’s horribly inaccurate review, this is a significant improvement.” (Diddier Prada, assistant professor of population health science and policy at the Icahn School of Medicine at Mount Sinai, was a co-author of the Baccarelli 2025 paper.)
The conflicting findings in Baccarelli’s paper and this paper by European researchers highlight the critical choices scientists make when designing a study. There is no perfect design that eliminates all confounding factors, especially when sifting through the countless variables that influence pregnancy and the historical omission of pregnant women from clinical trials.
Sibling control studies like those conducted in Sweden and Japan have become common in epidemiological circles thanks to a tantalizing promise: Having the same mother means that an association found between, say, Tylenol and autism will be free of the constant confounding factors between pregnancies, such as genetics, socioeconomic status, and more. If you have a large enough data set, you can address critical health questions.
Focusing on this specific type of differential exposure within a family has limitations, such as excluding families with only one child. This can also bias the results towards the null value, that is to say towards the absence of association between acetaminophen and certain disabilities. National Institutes of Health Director Jay Bhattacharya made these points when condemning sibling studies on social media in September.
But the limits cut both ways, said Jonathan Sebat, a professor of psychiatry and cell biology at the University of California, San Diego. Observational studies such as those favored in Baccarelli’s meta-analysis may overestimate the existence of an association. He said it is essential to use a study design that controls for genetic factors when autism is primarily hereditary, adding that it is difficult to summarily dismiss these sibling cohort studies when their accounting for genetic and familial confounding has not only weakened the association. He disappeared.
“This picture doesn’t really support the hypothesis,” Sebat said. “I need a lot more evidence now to really believe there is an association with acetaminophen.”
The myriad factors that influence child development can complicate a definitive statement, such as that Tylenol use does not cause autism or other neurodevelopmental disorders. But health experts say the latest review of evidence shows doctors should continue to use acetaminophen to treat pain and fever during pregnancy.
“This [study] “While the impact of last year’s announcement was significant, I hope the results of this study will help bring closure to the matter.”
Berita Terkini
Berita Terbaru
Daftar Terbaru
News
Berita Terbaru
Flash News
RuangJP
Pemilu
Berita Terkini
Prediksi Bola
Technology
Otomotif
Berita Terbaru
Teknologi
Berita terkini
Berita Pemilu
Berita Teknologi
Hiburan
master Slote
Berita Terkini
Pendidikan
Resep
Jasa Backlink
Togel Deposit Pulsa
Daftar Judi Slot Online Terpercaya
Slot yang lagi gacor